|
He argues that such answers are likely to be biased by extremes of experiences as well as being combined with more reflective judgements about the social context of their work. Kahneman argues that these types of questions (what he calls ‘attitudinal’ measures) require a respondent to summarise in one measure their experience of the job. 5 The UK Medical Careers Research Group (MCRG) survey asks questions such as ‘How much have you enjoyed the F1 year overall?’ or ‘How satisfied are you with the amount of time the F1 year has left you for family, social and recreational activities?’ 6 However, it is a single retrospective snapshot of experience in a single training post and more focused on issues in the system rather than individual factors. This has provided the wider system with an extremely rich source of data about the experience of training and patient safety in the UK. 4 The UK's General Medical Council has surveyed doctors in training for the past 10 years and achieved very high response rates. The standard method of capturing working conditions is to ask respondents directly. 1 Such working conditions not only result in poor or even dangerous care but could also contribute to the desire, by doctors in training, to leave the medical profession. High-intensity shift work, lack of breaks and inadequate sleep have all been posited as potential culprits. Levels of work-related stress and burnout among doctors are suggestive of harmful working conditions. 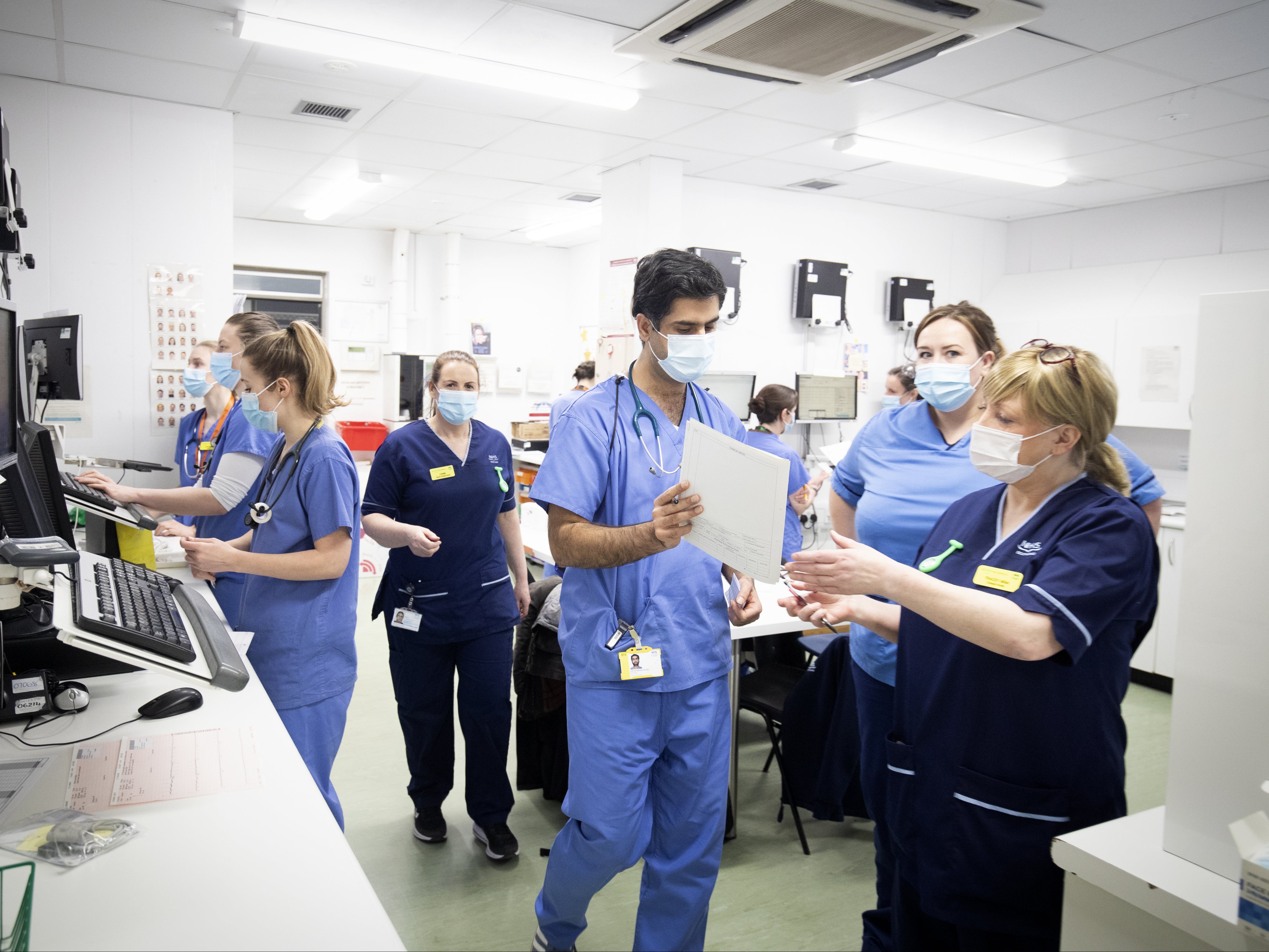
Educators and employers have important roles in recognising, advocating for and implementing improvements at work to enhance wellbeing with potential to improve retention of doctors in training. Systematic workplace changes (regular breaks, reducing paperwork and improved IT systems) could contribute to positive workday experiences and reduce intention to quit. Those having considered leaving the profession report more negative feelings. Positive emotions were expressed for breaks, staff meetings, research, learning and clinical tasks that involved patients. Respondents spent approximately 25% of their day on paperwork or clinical work that did not involve patients, resulting in more negative emotions. Consultations and negotiations for the next EBA will commence across 2020-2021.įor more information, contact Workplace Relations at or on (03) 9280 8722.Using an online tool, we report the association between tasks and ‘affect’ (underlying experience of feeling, emotion or mood) among 565 doctors in training, how positive and negative emotional intensity are associated with time of day, the extent to which positive affect is associated with breaks, and consideration about leaving the profession. During 2017-18, the AMA Victoria doctors-in-training subdivision was pivotal in its efforts to introduce improvements to the AMA Enterprise Agreement (EBA). Together, with AMA Victoria’s Workplace Relations team and the Australian Salaried Medical Officers Federation (ASMOF), doctors-in-training are a force for change. Moreover, we need the collective strength that a large membership provides to be able to negotiate improved workplace terms and conditions for all doctors in training in Victoria, and each additional member counts.ĪMA Victoria’s doctors-in-training subdivision is a powerful group of influencers responsible for driving huge improvements to workplace conditions. You must be a member of AMA Victoria for us to represent and support you in any individual workplace issue you may have. As a doctor-in-training, those reasons will be primarily related to workplace relations. There are many reasons why doctors join and stay members of AMA Victoria throughout their careers. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |


 RSS Feed
RSS Feed
